Mortality rates in Black and white Americans have been a significant area of concern in public health, revealing stark disparities that reflect deeper societal issues. While studies show that both racial groups are living longer, the divergence in health outcomes is particularly alarming among infants. Black infants face an especially troubling reality, as their mortality rates have worsened over the past 70 years, effectively doubling when compared to white infants. This raises critical questions about healthcare inequality and the effectiveness of public health policies that aim to address these racial health disparities. By understanding life expectancy differences and their implications, we can begin to advocate for equitable healthcare solutions that cater to the needs of all Americans.
Examining the differences in death rates between African American and Caucasian populations provides a crucial insight into the ongoing struggle against healthcare inequity. Recent findings indicate that while overall longevity has increased, the alarming rise in infant mortality rates among Black Americans highlights a troubling trend in racial health inequities. The significant gap in health outcomes invites a closer look at the factors contributing to these disparities, including access to quality medical care and the impact of socio-economic conditions. Furthermore, these statistics call into question the effectiveness of existing public health initiatives and policies that aim to mitigate such disparities. As we pursue solutions for healthier communities, it is imperative to address the complex layers that contribute to the disparities in mortality rates for different ethnicities.
Understanding Mortality Rates in Black and White Americans
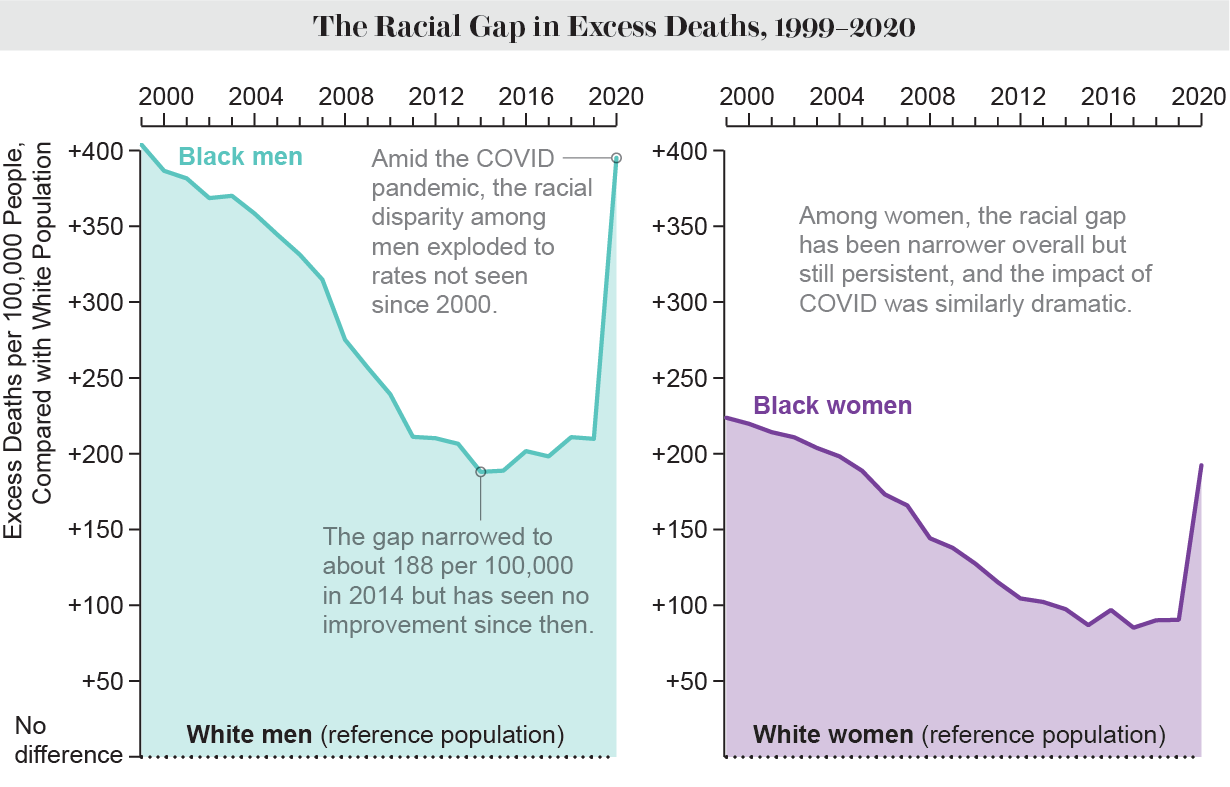
Mortality rates in Black and white Americans reflect significant disparities that persist despite overall improvements in life expectancy. Recent research indicates that, while adults in both groups are living longer—with life expectancy for Black Americans rising from 60.5 years in the 1950s to 76 years in the 2010s—the gap in mortality rates isn’t adequately closing for infants. Black infants have been observed to die at a significantly higher rate than their white counterparts, indicating a troubling trend that worsens over time. This stark difference presents a glaring inconsistency in healthcare outcomes and highlights the need for targeted interventions to improve health equity.
The statistics are alarming, with Black infants facing twice the mortality rate of white infants today. This trend has persisted and even widened since the 1950s, suggesting systemic issues within healthcare access and quality. Understanding these mortality rates is crucial not only in the context of public health policies but also in addressing racial health disparities that underpin these differences. The imbalance reveals deeper issues that go beyond health statistics, touching on socioeconomic factors, systemic racism, and healthcare inequality that plague communities across the nation.
Racial Health Disparities: Infant Mortality Rates
Infant mortality rates have long been a marker of health disparities, and the current data emphasizes a disheartening reality for Black infants. While there have been improvements in general healthcare over the decades, these advancements have not been equitably distributed. The recent findings designate medical conditions during pregnancy as a leading cause of excess deaths among Black infants, shedding light on the healthcare inequalities that exist before these infants are even born. This growing gap signals a failure in our health systems to provide equitable care and support for all families, especially those in marginalized communities.
Addressing the racial health disparities in infant mortality rates necessitates a multifaceted approach that includes not only healthcare access but also improved public health policies. Solutions must consider the broad spectrum of factors contributing to these disparities—ranging from maternal health education to enhanced prenatal care services. Strategic policy initiatives that target high-risk populations could significantly reduce the existing gaps, but this requires a commitment from both governmental and healthcare institutions to prioritize equity in health outcomes.
The Impact of Healthcare Inequality on Life Expectancy
Healthcare inequality affects not just infant mortality rates but overall life expectancy across racial lines. Although improvements in life expectancies have been noted in both Black and white populations, the persistence of an 18 percent higher mortality rate among Black adults highlights the systemic issues that still need to be addressed. The complexities involved include access to superior healthcare facilities, availability of preventative care, and socioeconomic factors that influence health outcomes. This illustrates the need for ongoing efforts to close the gap in life expectancy between these racial groups.
In examining life expectancy differences, it’s crucial to reflect on the historical context of healthcare disparities faced by Black Americans. Structural barriers, including but not limited to inadequate healthcare services, poor nutrition, and limited health education, continue to perpetuate these inequalities. Public health policies must be re-evaluated to ensure they effectively address the root causes of these discrepancies. Without a comprehensive strategy aimed at enhancing healthcare quality and access, the quest for equal life expectancy remains elusive.
Examining Public Health Policies and Their Role
Public health policies play a central role in shaping health outcomes and addressing disparities. The study highlights a significant gap in the effectiveness of policies aimed at bridging the mortality divide between Black and white Americans. While some progress has been made, particularly in adult health metrics, the widening gap among infants indicates that these policies often fall short. Policymakers need to prioritize research and data analysis to understand the unique challenges facing different demographic groups, allowing for the design of targeted programs that can mitigate these disparities more effectively.
Successfully addressing healthcare inequality will demand a holistic approach from public health authorities that integrates community-based initiatives with broader health system reforms. Initiatives could involve engaging with community leaders to foster trust and improve access to resources, incorporating cultural competency in care, and addressing the social determinants of health that deeply affect marginalized groups. Only through sustained, informed action can public health policies make meaningful strides toward health equity and improve outcomes for both infants and adults.
The Role of Socioeconomic Factors in Health Outcomes
Socioeconomic factors are fundamental in shaping health outcomes, particularly for racial and ethnic minorities. The disparities in mortality rates can often be traced back to differences in income, education, and access to healthcare resources. For instance, families with lower incomes may struggle to afford quality prenatal care, significantly impacting infant health. This relationship underscores the importance of integrating socioeconomic considerations into public health discussions and policy formulation, as these factors are pivotal in ensuring equitable healthcare access.
Moreover, healthcare inequality is exacerbated by the intersection of race and socioeconomic status, impacting Black families more severely. Disadvantaged communities often have limited access to quality hospitals, specialty care, and healthcare education, contributing to poorer health outcomes. A focus on improving socioeconomic conditions through policy reforms, education access, and economic support can play a critical role in enhancing community health and ultimately reducing disparities. Addressing these interconnected challenges is essential in the pursuit of health equity for all.
Looking Ahead: Bridging the Gap in Health Equity
Moving forward, bridging the gap in health equity must be at the forefront of public health initiatives. The alarming statistics surrounding infant mortality rates highlight the urgency with which these issues need to be addressed. With almost double the mortality rates for Black infants as compared to white infants, there is a clear indication that existing policies are inadequate. Increased funding for maternal health programs, community outreach efforts, and comprehensive education for healthcare providers could contribute significantly to improving this situation. Furthermore, establishing accountability measures within healthcare systems to ensure they are meeting the needs of all population segments is essential.
Moreover, as the nation continues to confront deep-rooted healthcare disparities, it is vital that community voices are included in the conversation. Empowering local organizations and groups that represent marginalized communities can provide valuable insights into the unique challenges they face and foster solutions that are culturally relevant. A collaborative approach that engages both community stakeholders and policymakers can lead to more effective strategies that truly address the factors fueling health disparities and work towards creating equitable health outcomes across the board.
The Urgency of Reforming Public Health Systems
The urgency for reforming public health systems has never been more pronounced, given the stark disparities highlighted by recent findings. With Black and white Americans experiencing contrasting mortality rates and life expectancies, it is evident that systemic reforms are needed. Focusing on equalizing healthcare access undoubtedly plays a key role, but it must also be accompanied by efforts to enhance the quality of care received by marginalized populations. This includes prioritizing public health initiatives that target the most vulnerable groups, ensuring they receive adequate support and resources.
In tandem with enhancing access, reforming public health systems will necessitate policy shifts aimed at root causes of health disparities. Addressing social determinants of health—such as housing, education, and environmental factors—must be integral to public health strategies. By implementing comprehensive reforms that consider these multifaceted issues, there is a greater chance for reducing disparities and ultimately improving health outcomes for all racial groups. It is a clarion call to public health institutions to act decisively and meaningfully in the quest for equity.
Seeking Solutions: Addressing Racial Disparities in Healthcare
The quest for solutions that address racial disparities in healthcare is ongoing, with many researchers calling for a multi-pronged strategy. An essential first step is recognizing the profound effects of structural inequality on health outcomes, particularly regarding infant mortality rates. Communities need resources, education, and access to health services tailored to their specific needs to envision equitable healthcare. This includes training healthcare providers in cultural competency to ensure they can effectively serve diverse populations.
Furthermore, collaborative efforts among healthcare providers, community organizations, and policymakers are vital in tackling the systemic causes of healthcare disparities. For example, initiatives that involve community health workers can bridge the gap in understanding healthcare access and resource utilization. By fostering collaboration and creating individualized support systems for communities, there is potential for tangible improvements in healthcare outcomes and a reduction in infant mortality rates among marginalized populations.
A Call to Action for Public Health Authorities
The findings regarding mortality rates among Black and white Americans signify a loud call to action for public health authorities. Immediate measures are needed to address the alarming mortality rates of Black infants, ensuring equitable access to quality healthcare for all. Health policy leaders must recognize that inequalities in mortality rates are not merely statistics but lives affected every day. Thus, concerted efforts must be put in place to enact policies that provide comprehensive prenatal care and education to expectant mothers in marginalized communities.
Additionally, this call to action obliges public health authorities to reevaluate existing frameworks and policies that may unintentionally perpetuate inequality. Regular assessments of healthcare disparities, alongside a commitment to listening to affected communities, can inform the development of more effective policies. By prioritizing the needs of marginalized groups and committing to true equity in healthcare, public health authorities can help ensure that future generations thrive and receive the care they rightfully deserve.
Frequently Asked Questions
What are the current mortality rates in Black and white Americans?
Mortality rates for Black Americans remain 18% higher than for white Americans. Overall, life expectancy has improved significantly for both groups, but disparities persist, especially for infants.
How do infant mortality rates differ between Black and white Americans?
Black infants have a mortality rate that is currently 115% higher than that of white infants, showing a widening gap since the 1950s when it was 92% higher.
What factors contribute to healthcare inequality affecting mortality rates among Black and white Americans?
Healthcare inequality stems from various issues, including unequal access to quality care, systemic racism, and socioeconomic factors that disproportionately affect Black Americans, contributing to higher mortality rates.
Why has the gap in infant mortality rates between Black and white Americans widened since the 1950s?
Despite improvements in overall life expectancy, the disparity in infant mortality rates has worsened due to persistent healthcare inequalities and factors such as medical conditions during pregnancy.
How have public health policies influenced mortality rates among Black and white Americans?
Public health policies have not sufficiently addressed the specific healthcare needs of Black Americans, particularly infants, leading to persistent disparities in mortality rates.
What does the study reveal about life expectancy differences between Black and white Americans?
The study indicates that life expectancy has improved for both groups, increasing from 60.5 to 76 years for Black Americans and from 69 to 79.3 years for white Americans over the past 70 years.
What measures can be taken to address racial health disparities in mortality rates?
Addressing racial health disparities requires targeted public health initiatives, improved access to quality healthcare, and policies tailored to eliminate systemic inequities affecting Black Americans.
Why is it crucial to understand mortality rates in Black and white Americans from a long-term perspective?
Long-term analysis reveals persistent inequalities that may not be evident in shorter studies, highlighting the need for sustained efforts and strategies to reduce health disparities over time.
How can future research influence public health policy regarding mortality rates among minorities?
Future research aimed at understanding the underlying causes of disparities can inform public health policies, ensuring that interventions are effectively designed to address the specific barriers faced by Black Americans.
What are the implications of the finding that 5 million Black American lives could have been saved with equal healthcare access?
This alarming statistic underscores the urgent need for policy changes and healthcare reforms that prioritize equity, ensuring that all Americans, regardless of race, receive the care necessary to improve health outcomes.
| Key Aspect | Findings |
|---|---|
| **Mortality Rates Overall** | Mortality rates between Black and white Americans have narrowed since the 1950s. However, Black Americans have an 18% higher mortality rate than white Americans. |
| **Infant Mortality Rates** | The disparity in mortality rates for infants has worsened, with Black infants dying at twice the rate of white infants today, compared to 92% higher mortality in the 1950s. |
| **Life Expectancy** | Life expectancy has improved for both Black and white Americans. For Black Americans, it increased from 60.5 years to 76 years, while for white Americans, it rose from 69 years to 79.3 years. |
| **Healthcare Disparities** | Healthcare inequality, including access and quality of care, significantly contributes to the disparity in mortality rates, especially among Black infants. |
| **Implications of Research** | The study analyzed data over seven decades, highlighting the persistent and worsening gaps in infant mortality rates. It calls for urgent public health attention to address these disparities. |
Summary
Mortality rates in Black and white Americans have shown improvements over the years, yet significant disparities, particularly among infants, persist. Recent research reveals that while life expectancy has risen for both racial groups, the gap in infant mortality rates has alarmingly widened, with Black infants facing much higher risks. This underscores the critical need for focused public health initiatives to address healthcare inequalities and improve outcomes for vulnerable populations. Reducing these disparities is not merely a goal; it is a moral imperative that requires immediate action.